Using End-of-Life Services
Understanding How End-Of-Life Unfolds for the Aged
Advance Directives
Palliative Care and Hospice Care
Choosing Where to Die
Assisted Suicide
When Death Occurs
Coping with the Loss of a Loved One
Final Arrangements--Preparing the Body
Funeral Services and Funeral Service Providers
The Cemetery, a Place for Memorialization
Pre-planned Final Arrangements with No Formal Funding
PreNeed (PrePaid) Funeral and Burial Plans
Checklists and Contact Information
Understanding How End-Of-Life Unfolds for the Aged
Cause of Death
No one in this country dies from old age. In the mid-1950s, "old-age" was discontinued as a cause of death on all US death certificates. The assumption was that old age itself was not a disease but contributed to life-threatening disorders that were the ultimate reason for death. The chart below shows the major causes of death for Americans age 65 and older. About 53% of those deaths are due to cancer or heart disease. But note also the high incidence due to stroke and chronic lung diseases.
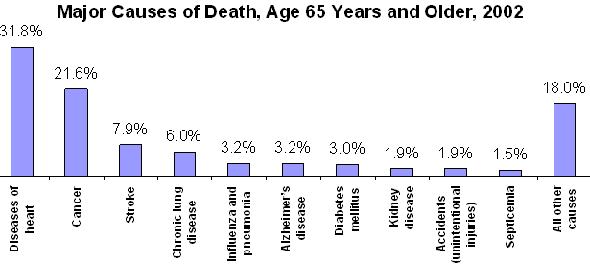
CDC, National Vital Statistics Report
Medical Care Prior to Death
In the first half of the 20th century most people who died had an accident or contracted a disease or had a physical disorder that quickly lead to death. Life-saving medical interventions such as sophisticated resuscitation, complicated surgeries, ventilators, feeding tubes and other life-support were rarely used or even available. Nowadays there is great emphasis on curing medical problems sometimes to the exclusion of recognizing that death might be a more welcome outcome.
Surveys indicate that older people are often more afraid of death than younger people. But for all Americans, young and old, there is a great fear of death and oftentimes family or those who are sick will go to great lengths to try procedures that may be ineffective in prolonging life. We need only look to the Terri Schiavo case as a reflection of the attitude of many Americans who are unwilling to let loved ones pass on. Estimates are that about 30% of Medicare reimbursements are spent on people in the last year of their life. It is a fact that much of this medical care did little to prevent death and prolong life.
According to the Dartmouth Atlas study on death:
"The quality of medical intervention is often more a matter of the quality of caring than the quality of curing, and never more so than when life nears its end. Yet medicine's focus is disproportionately on curing, or at least on the ability to keep patients alive with life-support systems and other medical interventions. This ability to intervene at the end of life has raised a host of medical and ethical issues for patients, physicians, and policy makers.
The Dartmouth Atlas project uncovered some startling differences in what happens to Americans during their last six months of life. In some parts of the country, nearly 50% of people are in the hospital at the time of death, rather than at home or in a nursing home or other non-hospital setting. In these areas, the likelihood of being admitted to an intensive care unit during the last six months of life is also higher than average - as is the likelihood of being admitted to an intensive care unit during the hospitalization at the time of death. In other parts of the country, the likelihood of a hospitalized death is far smaller, and people who are dying are much less likely to spend time in hospitals during their last six months of life.
The Atlas asked why this was so - why someone living in Miami was so much more likely to receive a great deal of high-tech, expensive medical services, while someone with the same condition who lived in Minneapolis received so much less. The answer appears to be that the capacity of the local health care system - the per-capita supply of hospital beds, doctors, and other forms of medical resources - has a dominating influence on what happens to people who are near death. Those who live in areas like Miami , where there are very high per capita supplies of hospital beds, specialists, and other resources, have one kind of end of life experience. Those who live in areas like Minneapolis or San Francisco , where acute care hospital resources are much more scarce, have very different kinds of deaths.
The question, then, is which is better? From the dying person's perspective, more is not necessarily a good thing - more visits to doctors for someone who is very sick can be stressful and exhausting. For many people a hospitalized death is something to be avoided if at all possible. From the perspective of the health care system, much of the care being given is futile, and accomplishes little. People who live in areas with very high utilization of hospital resources do not live longer than people who die in areas where utilization is lower - and if extension of life is not the goal of intervention, what is? From society's perspective, the cost of this kind of intervention is high, futile, and takes resources away from places where the money might be spent far more productively."
Deciding How and When to Stop Curing and Start Caring
Some people are content to leave decisions regarding their death in the hands of others. By doing so, they expose themselves to unnecessary and futile treatments as outlined above. They may experience numerous visits to the emergency room in the last stages of their life. And their dependency on others often results in great stress to family members when they lose their capacity and didn't make their last wishes known. Families are often forced to make decisions about life-support and treatment without knowing whether their loved one would have wanted these interventions.
Medical providers have come up against this situation many times and as a result there are written guidelines for doctors dealing with end-of-life issues. Here is a listing of official positions taken by the American Medical Association on a number of end-of-life actions.
Do-Not-Resuscitate Orders
Efforts should be made to resuscitate patients who suffer cardiac or respiratory arrest except when circumstances indicate that cardiopulmonary resuscitation (CPR) would be inappropriate or not in accord with the desires or best interests of the patient.Patients at risk of cardiac or respiratory failure should be encouraged to express in advance their preferences regarding the use of CPR, and this should be documented in the patient's medical record. These discussions should include a description of the procedures encompassed by CPR and, when possible, should occur in an outpatient setting when general treatment preferences are discussed or as early as possible during hospitalization. The physician has an ethical obligation to honor the resuscitation preferences expressed by the patient. Physicians should not permit their personal value judgments about quality of life to obstruct the implementation of a patient's preferences regarding the use of CPR.
If a patient is incapable of rendering a decision regarding the use of CPR, a decision may be made by a surrogate decision maker, based upon the previously expressed preferences of the patient or, if such preferences are unknown, in accordance with the patient's best interests.
If, in the judgment of the attending physician, it would be inappropriate to pursue CPR, the attending physician may enter a do-not-resuscitate (DNR) order into the patient's record. Resuscitative efforts should be considered inappropriate by the attending physician only if they cannot be expected either to restore cardiac or respiratory function to the patient or to meet established ethical criteria, as defined in the Principles of Medical Ethics and Opinions 2.03, "Allocation of Limited Medical Resources," and 2.095, "The Provision of Adequate Health Care."
When there is adequate time to do so, the physician must first inform the patient, or the incompetent patient's surrogate, of the content of the DNR order, as well as the basis for its implementation. The physician also should be prepared to discuss appropriate alternatives, such as obtaining a second opinion (eg, consulting a bioethics committee) or arranging for transfer of care to another physician.
DNR orders, as well as the basis for their implementation, should be entered by the attending physician in the patient's medical record.
DNR orders only preclude resuscitative efforts in the event of cardiopulmonary arrest and should not influence other therapeutic interventions that may be appropriate for the patient.
Futile Care
Physicians are not ethically obligated to deliver care that, in their best professional judgment, will not have a reasonable chance of benefiting their patients. Patients should not be given treatments simply because they demand them. Denial of treatment should be justified by reliance on openly stated ethical principles and acceptable standards of care, as defined in Opinion 2.03, "Allocation of Limited Medical Resources," and Opinion 2.095, "The Provision of Adequate Health Care," not on the concept of "futility," which cannot be meaningfully defined.Medical Futility in End-of-Life Care
When further intervention to prolong the life of a patient becomes futile, physicians have an obligation to shift the intent of care toward comfort and closure. However, there are necessary value judgments involved in coming to the assessment of futility. These judgments must give consideration to patient or proxy assessments of worthwhile outcome. They should also take into account the physician or other provider's perception of intent in treatment, which should not be to prolong the dying process without benefit to the patient or to others with legitimate interests. They may also take into account community and institutional standards, which in turn may have used physiological or functional outcome measures.Nevertheless, conflicts between the parties may persist in determining what is futility in the particular instance. This may interrupt satisfactory decision-making and adversely affect patient care, family satisfaction, and physician-clinical team functioning. To assist in fair and satisfactory decision-making about what constitutes futile intervention:
(1) All health care institutions, whether large or small, should adopt a policy on medical futility; and
(2) Policies on medical futility should follow a due process approach. The following seven steps should be included in such a due process approach to declaring futility in specific cases.
(a) Earnest attempts should be made in advance to deliberate over and negotiate prior understandings between patient, proxy, and physician on what constitutes futile care for the patient, and what falls within acceptable limits for the physician, family, and possibly also the institution.
(b) Joint decision-making should occur between patient or proxy and physician to the maximum extent possible.
(c) Attempts should be made to negotiate disagreements if they arise, and to reach resolution within all parties' acceptable limits, with the assistance of consultants as appropriate.
(d) Involvement of an institutional committee such as the ethics committee should be requested if disagreements are irresolvable.
(e) If the institutional review supports the patient's position and the physician remains unpersuaded, transfer of care to another physician within the institution may be arranged.
(f) If the process supports the physician's position and the patient/proxy remains unpersuaded, transfer to another institution may be sought and, if done, should be supported by the transferring and receiving institution.
(g) If transfer is not possible, the intervention need not be offered.
Quality of Life
In the making of decisions for the treatment of seriously disabled newborns or of other persons who are severely disabled by injury or illness, the primary consideration should be what is best for the individual patient and not the avoidance of a burden to the family or to society. Quality of life, as defined by the patient's interests and values, is a factor to be considered in determining what is best for the individual.Withholding or Withdrawing Life-Sustaining Medical Treatment
The social commitment of the physician is to sustain life and relieve suffering. Where the performance of one duty conflicts with the other, the preferences of the patient should prevail. The principle of patient autonomy requires that physicians respect the decision to forego life-sustaining treatment of a patient who possesses decision-making capacity. Life-sustaining treatment is any treatment that serves to prolong life without reversing the underlying medical condition. Life-sustaining treatment may include, but is not limited to, mechanical ventilation, renal dialysis, chemotherapy, antibiotics, and artificial nutrition and hydration.There is no ethical distinction between withdrawing and withholding life-sustaining treatment.
A competent, adult patient may, in advance, formulate and provide a valid consent to the withholding or withdrawal of life-support systems in the event that injury or illness renders that individual incompetent to make such a decision. A patient may also appoint a surrogate decision maker in accordance with state law.
If the patient receiving life-sustaining treatment is incompetent, a surrogate decision maker should be identified. Without an advance directive that designates a proxy, the patient's family should become the surrogate decision maker. Family includes persons with whom the patient is closely associated. In the case when there is no person closely associated with the patient, but there are persons who both care about the patient and have sufficient relevant knowledge of the patient, such persons may be appropriate surrogates. Physicians should provide all relevant medical information and explain to surrogate decision makers that decisions regarding withholding or withdrawing life-sustaining treatment should be based on substituted judgment (what the patient would have decided) when there is evidence of the patient's preferences and values. In making a substituted judgment, decision makers may consider the patient's advance directive (if any); the patient's values about life and the way it should be lived; and the patient's attitudes towards sickness, suffering, medical procedures, and death. If there is not adequate evidence of the incompetent patient's preferences and values, the decision should be based on the best interests of the patient (what outcome would most likely promote the patient's well-being).
Though the surrogate's decision for the incompetent patient should almost always be accepted by the physician, there are four situations that may require either institutional or judicial review and/or intervention in the decision-making process: (1) there is no available family member willing to be the patient's surrogate decision maker; (2) there is a dispute among family members and there is no decision maker designated in an advance directive; (3) a health care provider believes that the family's decision is clearly not what the patient would have decided if competent; and (4) a health care provider believes that the decision is not a decision that could reasonably be judged to be in the patient's best interests. When there are disputes among family members or between family and health care providers, the use of ethics committees specifically designed to facilitate sound decision making is recommended before resorting to the courts.
When a permanently unconscious patient was never competent or had not left any evidence of previous preferences or values, since there is no objective way to ascertain the best interests of the patient, the surrogate's decision should not be challenged as long as the decision is based on the decision maker's true concern for what would be best for the patient.
Physicians have an obligation to relieve pain and suffering and to promote the dignity and autonomy of dying patients in their care. This includes providing effective palliative treatment even though it may foreseeably hasten death.
Even if the patient is not terminally ill or permanently unconscious, it is not unethical to discontinue all means of life-sustaining medical treatment in accordance with a proper substituted judgment or best interests analysis.
Optimal Use of Orders - Not-To-Intervene and Advance Directives
More rigorous efforts in advance care planning are required in order to tailor end-of-life care to the preferences of patients so that they can experience a satisfactory last chapter in their lives. There is need for better availability and tracking of advance directives, and more uniform adoption of form documents that can be honored in all states of the United States . The discouraging evidence of inadequate end-of-life decision-making indicates the necessity of several improvement strategies:(1) Patients and physicians should make use of advisory as well as statutory documents. Advisory documents aim to accurately represent a patient's wishes and are legally binding under law. Statutory documents give physicians immunity from malpractice for following a patient's wishes. If a form is not available that combines the two, an advisory document should be appended to the state statutory form.
(2) Advisory documents should be based on validated worksheets, thus ensuring reasonable confidence that preferences for end-of-life treatment can be fairly and effectively elicited and recorded, and that they are applicable to medical decisions.
(3) Physicians should directly discuss the patient's preferences with the patient and the patient's proxy. These discussions should be held ahead of time wherever possible. The key steps of structuring a core discussion and of signing and recording the document in the medical record should not be delegated to a junior member of the health care team.
(4) Central repositories should be established so that completed advisory documents, state statutory documents, identification of a proxy, and identification of the primary physician can be obtained efficiently in emergency and urgent circumstances as well as routinely.
(5) Health care facilities should honor, and physicians use, a range of orders on the Doctor's Order Sheet to indicate patient wishes regarding avoidable treatments that might otherwise be given on an emergency basis or by a covering physician with less knowledge of the patient's wishes.
Treatment avoidance orders might include, along with a Do Not Resuscitate (DNR) order, some of the following:
• Full Comfort Care Only (FCCO);
• Do Not Intubate (DNI);
• Do Not Defibrillate (DND);
• Do Not Leave Home (DNLH);
• Do Not Transfer (DNTransfer);
• No Intravenous Lines (NIL);
• No Blood Draws (NBD);
• No Feeding Tube (NFT);
• No Vital Signs (NVS); and so forth.One common new order, Do Not Treat (DNT), is specifically not included in this list, since it may unintentionally convey the message that no care should be given and the patient may lose the intense attention due to a dying person; FCCO serves the same purpose without the likely misinterpretation. As with DNR orders, these treatment avoidance orders should be revisited periodically to ensure their continued applicability. Active comfort care orders might include Allow Visitors Extended Hours (AVEH) and Inquire About Comfort (IAC) b.i.d. (twice daily).
Surrogate Decision Making
Competent adults may formulate, in advance, preferences regarding a course of treatment in the event that injury or illness causes severe impairment or loss of decision-making capacity. These preferences should be followed by the health care team out of respect for patient autonomy. Patients may establish an advance directive by documenting their treatment preferences and goals or by designating a proxy to make health care decisions on their behalf.If an incompetent patient is to receive medical treatment, a reasonable effort should be made to identify the presence of an advance directive. When such a patient lacks a documented advance directive, or when reasonable efforts have failed to uncover such documentation, physicians should defer to state law to identify a surrogate decision maker. In the absence of state law specifying either appropriate surrogate decision makers or a process to identify them, the patient's family should become the surrogate decision maker. Family includes persons with whom the patient is closely associated such as close friends or unmarried living partners. In the case when there is no family, but there are persons who have some relevant knowledge of the patient, such persons should participate in the decision-making process. In all other instances, a physician may wish to utilize an ethics committee to aid in identifying a surrogate decision maker or to facilitate sound decision making.
When there is evidence of the patient's preferences and values, decisions concerning the patient's care should be made by substituted judgment. This entails considering the patient's advance directive (if any), the patient's values about life and how it should be lived, how the patient constructed his or her identity or life story, and the patient's attitudes towards sickness, suffering, and certain medical procedures.
In some instances, a patient with diminished or impaired decision-making capacity can participate in various aspects of health care decision making. The attending physician should promote the autonomy of such individuals by involving them to a degree commensurate with their capabilities.
If there is no reasonable basis on which to interpret how a patient would have decided, the decision should be based on the best interests of the patient, or the outcome that would best promote the patient's well-being. Factors that should be considered when weighing the harms and benefits of various treatment options include the pain and suffering associated with treatment, the degree of and potential for benefit, and any impairments that may result from treatment. Any quality of life considerations should be measured as the worth to the individual whose course of treatment is in question, and not as a measure of social worth. One way to ensure that a decision using the best interest standard is not inappropriately influenced by the surrogate's own values is to determine the course of treatment that most reasonable persons would choose for themselves in similar circumstances.
Physicians should recognize the proxy or surrogate as an extension of the patient, entitled to the same respect as the competent patient. Physicians should provide advice, guidance, and support; explain that decisions should be based on substituted judgment when possible and otherwise on the best interest principle; and offer relevant medical information as well as medical opinions in a timely manner. In addition to the physician, other hospital staff or ethics committees are often helpful to providing support for the decision makers.
In general, physicians should respect decisions made by the appropriately designated surrogate on the basis of sound substituted judgment reasoning or the best interest standard. In cases where there is a dispute among family members, physicians should work to resolve the conflict through mediation. Physicians or an ethics committee should try to uncover the reasons that underlie the disagreement and present information that will facilitate decision making. When a physician believes that a decision is clearly not what the patient would have decided or could not be reasonably judged to be within the patient's best interests, the dispute should be referred to an ethics committee before resorting to the courts.
Physicians should encourage their patients to document their treatment preferences or to appoint a health care proxy with whom they can discuss their values regarding health care and treatment. Because documented advance directives are often not available in emergency situations, physicians should emphasize to patients the importance of discussing treatment preferences with individuals who are likely to act as their surrogates.
A careful reading of the foregoing procedural positions from the AMA leaves a clear impression that health-care providers are looking for input from their patients or the patient's surrogates in treatment relating to end-of-life. Too often the patient or family simply let the system go into automatic mode and they do not assert their rights. It is extremely important for the medical community to know beforehand what the wishes of a person are concerning his or her medical treatment.
Advance Directives
One of the most important ways for a person to express his or her intent is through an advance directive. Advance directives for medical treatment ordinarily involve the four following written documents.
- Living will
- Health care treatment plan
- Health care power of attorney
- Do not resuscitate at-home (for states that allow a legal procedure for this action)
We will go into greater detail on these forms in the planning chapter but we will mention here some important points to consider with these documents. Many if not all healthcare organizations have standard forms for living wills. Some may also allow for signing a do-not-resuscitate order. A health care treatment plan is usually created between a patient's physician, the patient and an attorney. A health-care power of attorney is a legal document that would not usually be available as a standard form from a health-care provider. The do not resuscitate at-home arrangement is a very complicated procedure where a person needing emergency medical treatment in the home and not desiring resuscitation makes that wish known to emergency medical personnel. This involves an identification bracelet, a complicated verification procedure and an OK from a central clearinghouse not to perform any life-saving actions.
All too often a patient or his or her spouse or a family member will call 911 in the event of a life-threatening emergency. Almost never will the living will, the health care treatment plan or the health-care power of attorney end up with anyone in the emergency room. Without specific instructions, the emergency room will typically have the family sign a living will. But other health treatment wishes of the patient may be at home in the desk drawer. It is therefore extremely important to remember to take these documents to the emergency room whenever a crisis arises. If the patient has a do-not-resuscitate at-home legal arrangement -- for those states that allow such an arrangement -- and is not wearing his or her bracelet to identify this to emergency medical technicians, then it will be ignored and the EMTs will attempt resuscitation because that is what they are legally required to do.
Without the advance directives in hand for an emergency room or for a standard hospital admission many patients and family will be given the opportunity to sign a standard form from the health-care provider. Many hospitals, nursing homes and home health agencies have confusing, nonstandard living will forms that allow or disallow a number of treatments. It is extremely important for the patient or the family to read these institutional advance directives thoroughly before they sign them. We have seen a number of these documents that are both contradictory and confusing. Some of these documents claiming to be a living will, in effect, allow life-saving heroic efforts to be performed in contradiction to the principles of a living will.
Palliative Care and Hospice Care
Providing Comfort in a Facility or at Home
Palliative care is a new trend in medicine to provide comfort for the symptoms of the disease while not directly treating the disease itself. It is being used more and more in hospitals, nursing homes and by home health agencies to support the disease process. It is primarily used for people with severe illnesses and suffering from chronic pain, anxiety or discomfort.
Hospice is a form of palliative care for patients who are terminally ill. A commonly used definition for terminally ill patients is, "patients who have a progressive, incurable illness that will end in death despite good treatment, and who are sick enough that you would not be surprised if they died within six months." Whereas hospice comes into play when a patient is diagnosed as terminal, palliative care can be used at any stage in the treatment of a severe illness, from diagnosis on.
Because it is new, palliative care may or may not be covered by insurance plans such as Medicare. Or only certain protocols or medications might be covered. As it evolves so will the definitions, procedures and treatment plans. The concept involves a team approach using doctors, nurses, social workers and chaplains, similar to the hospice team. If a loved one is experiencing a great deal of discomfort or pain in the treatment process for a serious illness, the family should inquire whether the institution or care provider has a palliative care plan. Use of this care will help alleviate the suffering.
Hospice care has been around for 30 years and is a much better defined subcategory of palliative care. Hospice involves a team approach using the following providers.
- Family caregivers;
- The patient' s personal physician;
- Hospice physician (or medical director);
- Nurses;
- Home health aides;
- Social workers;
- Clergy or other counselors;
- Trained volunteers; and
- Speech, physical, and occupational therapists, if needed.
The purpose of hospice is the following:
- Manages the patient's pain and symptoms;
- Assists the patient with the emotional and psychosocial and spiritual aspects of dying;
- Provides needed medications, medical supplies, and equipment;
- Coaches the family on how to care for the patient;
- Delivers special services like speech and physical therapy when needed;
- Makes short-term inpatient care available when pain or symptoms become too difficult to manage at home, or the caregiver needs respite time; and
- Provides bereavement care and counseling to surviving family and friends.
A person can receive hospice from Medicare if he or she is
- eligible for Medicare Part A (Hospital Insurance), and
- the doctor and the hospice medical director certify that the person is terminally ill and probably has less than six months to live, and
- the person or a family member signs a statement choosing hospice care instead of routine Medicare covered benefits for the terminal illness, and
- care is received from a Medicare-approved hospice program.
A person may continue to receive regular Medicare benefits from his or her customary doctors for conditions not related to the hospice condition.
Although hospice is an outstanding service, Medicare does not pay enough or provide enough care for many patients. For those who have long-term care insurance, they may be able to get more hospice coverage from the insurance than from Medicare.
Pain Management
Pain management is the process of bringing pain under control. Pain can be a problem with many people at the end of life. Persistent pain can accelerate the decline in health due to poor nutrition, depression, lack of social stimulation and lack of exercise. And persistent pain becomes a form of disability, interfering in the ability to perform common daily tasks. Here is a list of problems that pain causes to one's self or to others:
- It is difficult to sleep
- It is difficult or impossible to pursue hobbies or personal activities
- Exhaustion can become a constant companion
- Depression is a very likely outcome
- There is little desire to eat
- It is difficult to enjoy the companionship of one's family
- There is reluctance to move about or exercise
- The patient and the caregiver become more isolated from the community because of the disability
- Family and friends who are caregivers become exhausted because of constant worry.
Chronic pain is a problem most often experienced by terminal patients who are dying from cancer. But non-cancer patients at the end of life may have other pain-causing conditions in addition to their terminal illness. This may be caused by such conditions as neuropathies, chronic back disorders or arthritis. Chronic or ongoing pain only adds to the suffering of a critically ill person. If the pain can be brought under control, a seriously ill patient can have a better quality of life for the remaining time available to him or her. Constant pain can also bring on depression which in turn could lead to suicide. Many people who cannot endure chronic pain take their own lives or seek out assisted suicide. Pain management may be a better alternative than suicide, not so much for the patient but more for the family. If a loved one takes his or her life, that can produce a permanent scar of shame or guilt within the family.
A major problem with persistent or chronic pain is that allowed to go on without treatment, the pain can become harder to treat. Research indicates that, over time, stimulation from persistent pain produces neural pathways in the brain that increase the intensity of the pain. In addition, pain receptors in the skin that are normally inert, may start transmitting sympathetic pain signals making the patient even more miserable. This can create a condition where a mere breeze or the wearing of clothing can be excruciatingly painful. Taking a pain pill occasionally as needed is not an effective treatment. Initially, it takes large doses of pain medication, on a regular schedule to bring the situation under control. Once the pain is under control, it is easier to maintain with continued lower doses of medication.
Sometimes people refuse to take strong pain medicine on a regular basis fearing dependency. But knowing that persistent pain itself becomes addictive should be incentive enough for people to seek treatment. Which is worse, addictive pain or reliance on medication? It is important to seek professional help with pain management and to establish an ongoing daily program to keep it under control. There are also numerous other non-drug techniques being developed for controlling chronic pain. Some of these might involve mind control techniques, acupuncture, electrical nerve intervention, massage or a host of other holistic approaches.
It is not necessary to refuse pain management because of a desire to display courage in dealing with terminal illness. A person is not a complainer because he or she admits to having pain. It is important to remember that caregivers are also susceptible to the stress of pain in their loved ones. The constant worry to the caregiver from ongoing suffering with the loved one will adversely affect the physical and emotional health of the caregiver. If not for themselves, persons experiencing persistent pain should seek their own treatment out of consideration for others who are concerned about their welfare.
The most common line of treatment in pain management is the use of medications. Here is a list of medications commonly used with three levels of pain.
- Mild pain - For mild cancer pain, acetaminophen or nonsteroidal anti-inflammatory medications (NSAIDs), such as ibruprofen, are often used.
- Mild to Moderate Pain - For mild to moderate cancer pain, when pain relief is not achieved with acetaminophen or NSAID medications, opioid medications are often used, usually as combination tablets with NSAIDs or acetaminophen. Some of the opioid medications used as combination products are hydrocodone, codeine, or oxycodone. Adjuvant medications may also be used for pain that is difficult to manage. Adjuvants are medications that were originally designed to treat conditions other than pain, such as tricyclic antidepressants.
- Moderate to Severe Pain - Moderate to severe pain is usually best treated with higher doses of opioid medications often not given as combination products. Adjuvant medications, NSAIDs, and acetaminophen may also be used. The opioid medications used to treat moderate to severe pain include morphine, fentanyl, oxycodone, and hydromorphone.
If the attending physician does not seem to know much about pain management or is unwilling to provide a referral to a pain clinic, the patient or caregiver need to take matters into their own hands to bring the situation under control. Referral from a friend or a listing in the Yellow Pages can lead to specialists who can help.
Choosing Where to Die
Birth and death are consequences of life. They happen to every one of us. Where birth is often a joyous occasion, death is often a sad occasion. But it not need be. It is hard to let go of someone we are close to but death also releases the loved one from pain, anxiety and unhappiness. For a caregiver, death is a welcome relief from years of sacrifice, stress and financial burden. And for those who believe in a life after death, a loved one has been released from a life of burden to a life of happiness.
Regardless of religious belief, the death of a loved one can often be a spiritual experience. But dying in the wrong setting can often lead to the departure of a loved one being an upsetting experience for the family. When a person expires, at peace in his or her own home, in a familiar setting and surrounded by loving family, that death can be an experience that the family cherishes forever. When a person dies in a hospital or nursing home amid the confusion of busy workers, tied to tubes and noisy machines and agitated by the lack of a familiar setting, that death may be remembered as an unsavory experience.
A recent survey by the End-of-Life Care Partnership, a Utah nonprofit end-of-life support group, sheds some additional light on the preference of Utahns where they would have chosen to die. A random phone survey of 150 survivors of recently deceased people was conducted. The deceased ranged in age from 23 to 100 but the mean age was 74 and over 75% of those who died were 65 or older. Over 80% of the respondents were spouses or children with the remainder having some other relationship to the deceased. The chart below indicates where the decedent's actually died.

About 54% of the subjects died where they wanted. This means the other half of the group was denied their preference of their place of death. Those who were 65 or younger more often died at home (55%) and 97% in this group preferred their home as a place of death. Of those over 80, 38% actually died in a nursing home whereas 76% of those over 80 wanted to die at home. Comparing their last desires to where the study group actually died indicates we are doing a very poor job in meeting the end-of-life wishes for terminally ill patients. The study also compared these results to national statistics reporting where death occurs and found that people from Utah died more frequently at home than people nationally. Also studies done nationally indicate that those who are currently living, predominantly would prefer to die in their homes.
The person who is dying can choose the setting if he or she wants. There is no reason to die in an institution unless there is little time to transport the person to a more familiar environment or unless a person specifically wants to die in a facility. A person who is cognizant always has complete control over the medical care he or she receives. If the person who is terminal cannot make such a decision, then the family can. There is no reason for anyone to accept death in an environment not of his or her choosing. Too often people accept the situation and don't act aggressively in making their needs known. Too often for a loved one at home, who is dying, and who is in crisis from pain or other acute attack, calling 911 becomes the first option. The loved one in crisis is transported to a hospital where death may occur. With proper planning a crisis need not result in transportation to a hospital emergency room.
Palliative end-of-life care is now a commonly available alternative for people at home who are in the last stages of their life. This could be hospice or some other form of palliative care. A crisis under palliative care would result in a call to the attending nurse or doctor and based on prior arrangements or advice, the crisis would be handled without calling an ambulance. We recommend that all terminally ill patients and their family make planning for death, using palliative care, a routine part of the preparation for the end of life.
Assisted Suicide
Our purpose in discussing this subject is not to pass judgment or to create controversy but simply point out that there is a growing movement for people to end their lives in order to avoid suffering from a debilitating terminal illness. And people seeking assistance of others, primarily the medical profession, to help them take their lives is becoming more common.
Assisted suicide basically hinges on a religious debate as to whether suicide is morally right or wrong. Those who profess no religious foundation for their actions may not see a moral problem with assisted suicide. There is however the legal issue which makes it unlawful in all states except for Oregon . Oregon has had an assisted suicide law on the books for a number of years.
Other cultures will condone suicide under certain conditions. For instance in Japan a person can take his life to protect his honor. It appears that in Muslim culture, suicide is a noble act when one destroys enemies in the taking of one's life. But even in our society, suicide is forgiven when a person sacrifices himself for the greater good of saving others.
Here is the position of the American Medical Association on allowing a member of the medical profession either assisting someone to take his or her life or in an act of compassion -- called euthanasia -- taking that life without permission.
Euthanasia
Euthanasia is the administration of a lethal agent by another person to a patient for the purpose of relieving the patient's intolerable and incurable suffering.
It is understandable, though tragic, that some patients in extreme duress-such as those suffering from a terminal, painful, debilitating illness-may come to decide that death is preferable to life. However, permitting physicians to engage in euthanasia would ultimately cause more harm than good. Euthanasia is fundamentally incompatible with the physician's role as healer, would be difficult or impossible to control, and would pose serious societal risks.
The involvement of physicians in euthanasia heightens the significance of its ethical prohibition. The physician who performs euthanasia assumes unique responsibility for the act of ending the patient's life. Euthanasia could also readily be extended to incompetent patients and other vulnerable populations.
Instead of engaging in euthanasia, physicians must aggressively respond to the needs of patients at the end of life. Patients should not be abandoned once it is determined that cure is impossible. Patients near the end of life must continue to receive emotional support, comfort care, adequate pain control, respect for patient autonomy, and good communication.
Physician-Assisted Suicide
Physician-assisted suicide occurs when a physician facilitates a patient's death by providing the necessary means and/or information to enable the patient to perform the life-ending act (eg, the physician provides sleeping pills and information about the lethal dose, while aware that the patient may commit suicide).
It is understandable, though tragic, that some patients in extreme duress-such as those suffering from a terminal, painful, debilitating illness-may come to decide that death is preferable to life. However, allowing physicians to participate in assisted suicide would cause more harm than good. Physician-assisted suicide is fundamentally incompatible with the physician's role as healer, would be difficult or impossible to control, and would pose serious societal risks.
Instead of participating in assisted suicide, physicians must aggressively respond to the needs of patients at the end of life. Patients should not be abandoned once it is determined that cure is impossible. Multidisciplinary interventions should be sought including specialty consultation, hospice care, pastoral support, family counseling, and other modalities. Patients near the end of life must continue to receive emotional support, comfort care, adequate pain control, respect for patient autonomy, and good communication.
The AMA does not condone such actions and the statements imply that a physician engaged in such practice would be committing an undesirable act not in keeping with the purpose of medicine. But notice also that the AMA does not prohibit such activity.
This leaves open the possibility that medical professionals living in a state where euthanasia under certain circumstances or assisted suicide might be legal, could engage in such a practice if they chose to.
The biggest problem with using suicide to avoid prolonged suffering at the end of life is the effect it has on family. If there is no family or the family has been consulted and is at peace with such a decision, then suicide might be acceptable. But our society does not generally except suicide and for someone to take his or her life willingly could be a great psychological blow to the family. The stigma, guilt and shame a family may carry from someone committing suicide could cause emotional wounds in family members for the rest of their lives. Anyone, not suffering from severe depression--which can cloud rational thinking, should be counseled to consider the consequences of suicide before using it as an option to avoid the distress of an unpleasant natural death. The person contemplating suicide may not know of options other than suicide, such as treatment for depression and hospice care and pain management.
When Death Occurs
When a loved one dies at home, family or others who are there must often cope with the reality of the dying process. We recommend strongly that when a person is first considered being terminal, the doctor should be asked to order hospice care. We cannot stress enough how hospice care can help those involved get through a death at home or even in a care center. Oftentimes the family waits until a loved one is well along towards the end of life before hospice is considered.
Hospice is generally used for cancer patients because it is often easy to determine in advance whether a person will survive or not. If the cancer is not cured and continues to spread, death is usually inevitable. Whether that occurs in a matter of weeks or months is not important to the doctor prescribing hospice. The only requirement is the doctor must have a reasonable expectation that his patient cannot survive beyond six months. Sometimes hospice patients can receive care for years before they succumb.
For other medical conditions hospice may be just as appropriate but oftentimes the family fails to inquire or the family doctor simply doesn't consider it. Hospice should be considered for such conditions as congestive heart failure, advanced diabetes, advanced lung disease, advanced autoimmune disorders, advanced kidney disease and so on. Even in the absence of any medical condition, a person can still qualify for hospice if he or she is deteriorating rapidly and overall health is declining. Another condition often overlooked for hospice is advanced dementia or Alzheimer's disease. Family often waits until a loved one starts shutting down before hospice is ordered. Or sometimes hospice is not even considered for Alzheimer's because doctors are so used to using palliative care only for cancer. If a loved one is not improving, family should always ask or even press for hospice. Remember not to wait until close to the end but order hospice at an earlier stage since it will help provide the necessary transition to the death of a loved one.
Why are we so adamant about using palliative care? Because these services focus on dying patients and will help the family get through not only the death but also give physical and spiritual comfort to the person dying as well as offering bereavement support after the death. We simply can't stress enough the importance of using this type of support when the end is near.
When a person is close to death, physical changes occur. Blood flow slows down and fingers and toes may start turning blue or black. Breathing is labored, there is a rattling at the back of the throat and the breathing process may even cease for long periods and then resume again. A loved one will be cold and it is important to provide blankets for warmth. A loved one may be confused or he or she may simply sleep a lot. Since these changes will be noticeable to the caregiver, a call to the hospice will receive immediate response with either a visit or instructions over the phone.
Remember hospice is on call 24 hours a day and the service is there to provide exactly this kind of support when death is imminent. Because of this support, the caregiver and other family members will be able to spend more quality time at the bedside of their loved one. Their fears for their loved one will be dealt with by a staff that can be relied on for knowing exactly what to do. Supportive services with the death of a loved one can make a huge difference in the way family handle the consequences of the death.
After death occurs, the hospice workers will also make arrangements for a funeral home to pick up the body. They will also help clean up any soiled bedding and talk to the attending physician about other follow-up, say an autopsy.
Coping with the Loss of a Loved One
Understanding Bereavement, Grieving and Mourning
Bereavement or grieving is the process and period of time during which someone suffers grief from the loss of a loved one. Mourning is a public display of grief. In our culture, mourning is not an officially prescribed ritual except perhaps for certain religious groups. In other cultures it can become a prolonged public display lasting for many days or even many weeks. This might include multi-day public wakes, the use of professional mourners, the wearing of black attire, remaining sequestered in the home or the prescribed use of religious rituals.
Grief is a condition experienced by all where someone suffers a loss of another person who is close. When we love someone and they die, the feeling of loss can often become an overpowering experience. It is almost like a part of us has been torn out and we can't cope with the feelings it brings upon us. Grief is a normal part of our human experience. As human beings, we work together and rely on each other as a part of our existence. Human culture could not exist without this inter-cooperation. This reliance on others, especially someone we love, becomes over time intertwined into the function of our brain. When a loss occurs, our mental process must physically readjust to a new reality and the period of grieving is the process we go through to retrain our minds.
Even though no one really ever completely recovers from the loss of a loved one, most of us tend to find strategies that allow us to push it into our distant memory. It lingers there and we can retrieve it from time to time but it does not evoke the same powerful emotional response it once did. On the other hand, some people simply never deal with the emotions of grief and it remains in the forefront of their minds for a long time if not forever. This can have a powerful disabling effect on a person and may prevent that person from leading a normal life. It is extremely important to learn to deal with grief not only for personal reasons but for the sake of other loved ones who are still alive.
The intensity of the grief experienced and the subsequent ability or inability to deal with it are often a result of the nature of the loss itself. When a death is anticipated from a long illness or because of extreme old age it is often easier to deal with than an unexpected death. The time between knowing that death will come and the actual death allows for the grieving process to take place in advance. A spouse, children or other close people will rehearse in their minds many times over what will happen when a loved one is gone. This helps prepare them for the day it will happen and often shortens the grieving period. On the other hand, even with an anticipated death, sometimes two married people are so close that when one dies the other is completely lost and never fully recovers. It's not surprising when the survivor dies soon after.
The most difficult death to deal with is a sudden death involving violence or a suicide. Not only is the unexpected event a shocking experience but the nature of the death also leaves the survivors feeling violated, guilty and unprepared. Normally deaths of this type require professional assistance from a counselor to help the living cope with the extreme grief such a death can cause.
There is no timetable for bereavement. Every person deals with it in his or her way. For some the process requires but a few weeks and they can go on with their life as before. For others it may take years. And for some grief becomes a chronic daily burden and if that person doesn't deal with grief then it can prevent one from living. Also chronic grief often results in depression. If the intensity of the grief does not diminish and there are problems with eating, sleeping, continuing feelings of guilt or the inability to function, professional assistance is needed.
Managing the Grieving Process
Some authors like to break down the grieving process into stages. The reason for this is so that those grieving can recognize if they are making progress towards resolving their grief. Recognizing the various emotions associated with the process will help a person determine at what stage they are. Here is one author's dichotomy.
Disbelief
Almost everyone has difficulty accepting a loss. Most people simply want it to go away as if it never happened. They will tell themselves such things as "why me?", "why can't I start over?", "this seems like a bad dream" and so on. Their thinking is numb and they want to forget it, but in the back of their minds there is a deep foreboding of what happened. They can't shake the reality of their experience.Reaction
After the initial shock has worn off and there can be no more denial then there must be a reckoning. Some will express anger. Some will blame others. Some will retreat and become brooding and stoic. Each person has his own way of reacting to a loss.Sorrow
When striking back at a loss no longer seems an acceptable strategy, and then sorrow sets in. A person might feel sorry for himself or for others or both. A great deal of tears are normally shed and it is at this stage that one seeks comfort from others. The person in mourning may also find it difficult to do anything or to talk to anyone. Family or friends should recognize that comfort is being sought, regardless of the attitude of the person in mourning, and offer their support. But sympathy may not always be the best strategy. Encouraging activity and involvement in other things might be a better way to support someone in grieving.Acceptance
At some point most people who have lost a loved one have worked through their emotions and no longer have the need to be angry or to feel sorrow. Those emotions may still be there but they are placed in the back of the mind and a concerted effort must be made to relive them. Otherwise they seem as a wisp of smoke, something seen but not recognized.
Some People can work through bereavement very quickly and resolution comes within a matter of days or weeks. They readily accept the loss, work through their anger and sorrow and are ready to move on. Unfortunately some people get stuck in one phase of the process. They may spend considerable time in denial. They may spend months or even years being angry. Or they may have gotten past the anger and they are preoccupied continually with feeling sorry for themselves.
In fact this is the test that one uses to determine if the grieving process is spent. If a great deal of one's waking moments are spent on rehashing what could have been (disbelief) , working on strategies of "getting even" (reaction) or allowing thoughts of the loss to interfere with daily life (sorrow) , then a person is not through the grieving process. By stepping back and looking at oneself as if from someone else's eyes and then recognizing the problems we have just discussed, a person in grieving can then make a decision about what to do next. This may involve seeking help from family or friends or it may involve the services of a professional counselor.
Grieving and depression are not the same thing. Prolonged grieving, however, can often lead to depression. And as we have discussed previously, depression is a major contributor to suicide in older Americans. The suicide rate of the elderly is about four times that of the rest of the population. It is therefore very important to avoid depression with the loss of loved ones. Grief may manifest symptoms similar to depression such as sleeplessness, loss of appetite or a feeling of gloom but unlike depression, grief can be set aside. One way to recognize the difference is if engaging in physical or mind stimulating activities results in the gloom going away, at least for that period of time, it is unlikely to be depression. Depression does not go away regardless of what one does.
As a general rule the grieving process is a mental process that can be overcome by retraining one's thinking. Depression on the other hand may have resulted from improper thinking but it has become a physiological problem with an imbalance of chemicals in the brain. The brain itself is not working correctly. Depression is much harder to treat. It may require medications or it may respond to cognitive therapies but the intensity of those therapies is much deeper than what one would need to work through a grieving issue.
When a person feels he or she cannot cope by themselves with grief or the potential of depression it is time to seek help. It is important for family or friends to realize that many people can't recognize by themselves they have a problem. Especially those who have become depressed. Depression creeps up over a period of time and results in mood changes and changes in thinking patterns that the afflicted person may not recognize have happened. A person with depression often feels he is "normal" and will even resist someone telling him that there might be a problem.
For mild problems or those a person readily admits to having, it may not be necessary to bring in professional help. Here are some strategies borrowed from the web site "helpguide.org" at https://www.helpguide.or.
"Death is part of life; hanging on will not prolong your loved one's life or bring them back. Letting go and surrendering to the grieving experience, with the help of others, will bring comfort and solace. Here are some other areas in which you can 'grieve well':
• Self-expression
• Physical self-care
• Emotional self-care
• Good social support
One of the key elements of healthy grieving is allowing your emotions to surface in order to work through them. In the long run, trying to stuff down your feelings-in the belief that they will simply fade with time-is counter-productive. When ignored, grief causes pain that is sometimes so excruciating that people want to numb and escape it through alcohol or medications. But in blocking the grieving process you block the natural return to interest and meaning in life that follows the grieving process and is its real end point.
Take care of yourself through self-expression
• Talk. You deserve to express yourself at this difficult time, even though others may discourage or even reprimand you for having a strong emotional reaction. Talk about your loved one to others or to God (and encourage them to do so, too). If they are uncomfortable, gently let them know that part of your healing process is getting it off your chest.
• Write. Start or continue writing in a journal or diary. You may want to compose a letter to the deceased person to describe how you feel and 'say' things you never got to say. Some questions to write about: how would you spend the rest of your life if you only had a short time to live? Would you say or do things differently? Be as honest as possible about how you feel.
• Create. You may want to create a special collage or other artistically-inspired memento about your loved one, like a scrapbook. For those who are beginner artists, you can use memorabilia items or something symbolic like seashells. In the process, your thoughts and feelings may become clearer as you provide a creative outlet for expression. This exercise also may bring up other feelings that you need to face.
• Remember . Let this be an opportunity to reflect on the good times. Looking back, what do you appreciate about the contributions of your loved one? What are the moments together that you cherish the most? Do things to honor and remember your loved one: if they loved flowers, plant a garden in their honor or help others plant gardens; support the causes and organizations that were important to your loved one.
Take good physical care of yourself
• Get enough sleep . A regular sleep routine will be of benefit. If you are tired during the day, give yourself a chance to sit or lie down. Resting your body will help your emotional recovery. See Helpguide's Getting the Sleep You Need: Sleep Stages, Sleep Tips and Aids to understand why a restful night's sleep is important and how it's adversely affected by caffeine, medications, heavy smoking and alcohol.
• Avoid chemicals. Though you may crave a chemical to help you get through this time, try your best to steer clear of substances like alcohol, caffeine, nicotine, because their side effects can be unhelpful in the long-term. For instance, instead of coffee, opt for green tea, which is less jolting to your energy.
• Exercise regularly. If you are physically able, take a brisk walk in the morning or at lunchtime. Choose something that will motivate you to get out of bed. For more tips on how to begin an exercise routine no matter what your age, see Helpguide's Senior Fitness and Sports . Whether you feel like it or not, get some sort of physical exercise every day.
• Eat well . Even if it's the furthest thing from your mind, pay attention to the quality of what you eat. Take the time to eat nutritious meals while sitting down, avoiding processed or 'fast' food (even though you may be pressed for time and not feel like cooking). For more information on optimal nutrition, especially when you must eat out, read Helpguide's articles on Healthy Eating: Guide to New Food Pyramids and Tips for a Healthy Diet and Healthy Restaurant Eating / Fast Food Nutrition: Guide to Making Healthy Choices .
Take care of yourself emotionally
• Have fun. Is there a book that you have wanted to read or a movie you haven't had time to see? This is the time to do it. Whether it's listening to uplifting music or getting a massage, do what makes you happy. For more ideas, see Helpguide's Playing Together for Fun: Creative Play and Lifelong Games . Even though you may feel guilty about being pampered at this time, you deserve to treat yourself well.
• Forgive. The death of someone you love brings an end to opportunity to communicate. You may be reminded of the need to forgive that person for a past hurt-and forgive yourself if need be-then move on. Maybe you said something you regret. Perhaps you wish you had done more at the time. In your grief, you may have felt embarrassed, guilty or angry (which is completely understandable). Let yourself off the hook and apply that energy into something positive.
• Plan ahead. Anniversaries and holidays bring their own particular challenges. You may feel especially emotional a year after your loved one dies, on their birthday or another significant marker. Attending an event such as a graduation, wedding or funeral can be highly charged, as well. This is a completely normal reaction. In order to prepare, talk to other members of your family to find out what their expectations are. Decide together how you would like to change your traditions while honoring the memory of your loved one.
• Get the support you need. There are people who want to help you get through this time-friends, loved ones, pastoral counselors, bereavement counselor, trained laypersons and professionals .Often people want to help, but don't know what to do.
• Accept help that feels good.
• It's alright to tell people who want to help how they can best help you.
• One of the most helpful things might be to prepare healthy meals for you.
• Some people can take time to just listen and hold you as you cry.
• A good friend might even laugh with you, in the midst of your pain.
It is important to have an outlet for sharing grief, even for people who aren't usually comfortable talking about their feelings. Humans are social creatures and knowing that others know and understand will make you feel better, less alone with your pain. Many support groups exist for the general public as well as specific populations, such as grieving parents and suicide survivors. Whatever the nature of your loss, connecting with others will help you heal. You will know how far you've come when you can share another's pain and know the possibility of recovery."
For those needing professional help there are two types of therapy. The first is called grief support. Grief support may simply consist of talking through issues with a counselor and recognizing the faulty thinking and implementing corrective strategies. Or it may involve group sessions with people in a like situation, again with the idea of coming away with strategies to deal with the grief problem. Grief support can be found by contacting a local hospice agency as these people specialize in helping their clients through the bereavement process.
The other therapy is called grief therapy or grief counseling. This usually involves sessions with a trained therapist to resolve underlying issues. Grief therapy is often needed when a person is dealing with very intense grieving issues. This may be a loss of a loved one in an accident or a murder or through suicide. Such losses can be so traumatic that people can't get through them themselves and require professional help to deal with it. For example, grief therapy is an automatic response for students who might experience a fellow student dying in a tragic accident, taking his or her life or using firearms in the school to take the lives of others. Grief therapists are going to be licensed therapists, psychologists or psychiatrists specializing in this practice.
Final Arrangements -- Preparing the Body
In the early days of our country when a person died, members of the community would come together, wash the body, clothe it and prepare it for burial. Then often members of the community or family would pay their respects by coming to the home of the deceased for a viewing. Finally, a day or two later, there might be a funeral service followed by a burial. There were no fancy caskets, no embalming (except for a period after the Civil War) and no cemetery vaults. The practice of burning a body after death in a furnace or funeral pyre was not generally done. As a consequence of our history, our culture has become accustomed to preserving the body for burial. This is not necessarily true in other cultures. Hindus and Buddhists almost always cremate their loved ones.
The period of time between interment in a mausoleum or burial in the ground could be as much as a week or more, owing to the need to notify members of the family who are living far away, allowing them to travel to where the interment will take place and allowing time to make arrangements to buy burial plots and so forth. Nowadays, funeral homes and undertakers usually have refrigerators to preserve the remains while arrangements are being made. Also it is common tradition to have a viewing either a day or two before the burial or funeral or just prior to burial or funeral.
Embalming is a common practice in the United States and Canada but is generally not as popular in the rest of the world. For some, embalming is a way of providing respect by retarding the natural decay of human flesh. For others and for certain religions embalming is considered a desecration of the body. Studies done at the University of Tennessee reveal that all bodies decompose, embalmed or not. It just may take longer for the embalmed body to return to the earth. Embalming fluid may also contain dye to make the skin look more lifelike. The embalming process also allows for funeral home workers to safely "restore" the body by repairing injuries, filling out the face through padding, forcibly closing the jaw, injecting collagen and using cosmetics to make the deceased appear "natural", as if he or she were slightly younger and in good health. It is also traditional to dress the loved one in formal or favorite attire. Families appreciate seeing their loved ones in a favorable light. It helps them remember the departed one in a pleasing setting. A common phrase used by those filing through a viewing is "He/She looks so good!" On the other hand, lifelike viewings are sometimes disturbing to people as well.
Embalming and restoration are not a necessary process if there is no viewing or for that matter even if there is a viewing. Even though viewings would be safe without embalming, very few funeral homes will consent to viewing without the process. In many states there are no laws requiring embalming except if bodies are transported across state lines, shipped internationally or shipped commercially. It is never required for the first 24 hours in any state; 22 states require embalming after 24, 48, or 72 hours, but refrigeration is usually an alternative option. (Refrigeration is not an option in Alaska , Minnesota or North Dakota. ). Under certain circumstances, medical examiners may require embalming pursuant to an investigation or if death were due to contagion. Due to the use of refrigeration, the remains can be transferred to a coffin for a funeral or graveside service without incurring this additional cost. For funerals and viewings conducted in the home, dry ice is often used to retard decomposition.
The cost of embalming and restoring as well as the cost of expensive coffins and vaults can be avoided by using cremation. Cremation is typically a much less expensive process and some families prefer it to keeping the body in its natural state. It is also a simpler process as far as making arrangements for viewings and services if such services are not desired. Since a funeral and interment can often be the third largest expense a family can incur after purchase of a home or a car, many families simply must find a less expensive way to provide final arrangements for loved ones. Some don't have the money for expensive services but still want to provide respect for a decedent and not simply put them in a pine box and place them in the ground. For these reasons and many others cremation is becoming more popular. Estimates are that 20% to 30% of all last arrangements use cremation.
It is interesting to note that legally in more than half of the states; the deceased person has no postmortem rights to what happens with his body. In those states, the family does what it wants, although many times the wishes of the departed are respected if that person made his or her wishes known before death or has created some binding condition in a will that forces the family to comply. If the decedent wanted a traditional burial, the family may choose cremation. If the decedent wanted cremation, the family may choose a traditional burial.
What is often not understood about cremation is that it does not prevent having a funeral or graveside service or even burying the remains in a grave. The body is still there, it is just in another form. In fact a traditional viewing and funeral service can even be arranged before the cremation takes place. If the family does not want to purchase an expensive casket for a pre-cremation, traditional service, a casket can be rented. Family may also view the cremation process. In most states there must be a waiting period before cremation can occur, for legal purposes, since there is no way to identify cause of death after cremation. Also some states require permission from a medical examiner or corner for the same reason. If it is a suspicious death, obviously cremation will not be allowed.
The process consists of first removing a possible heart pacemaker and external metal objects from the body and then it's common to place it an inexpensive wooden or cardboard coffin. But needing a coffin for cremation is not always required and simply adds to the expense. The body and or coffin are placed in a very hot furnace until everything is reduced to ash. This takes several hours. There may be remnants of metal parts such as artificial joints and there may remain a few pieces of bone. The metal parts are removed and the ashes and bone are processed to a very fine powder. The family has chosen beforehand a suitable receptacle or urn and the ashes are placed in it. The family can choose to have a funeral, a memorial service, or nothing at all. The ashes can be placed in a mausoleum in a cemetery, they can be buried in a cemetery plot, they can be kept in someone's home or they might be scattered in a suitable location.
Services centered on a cremation can be considerably less expensive than traditional funeral services. It is estimated that the average cost of a funeral in the United States is about $8,000. Interment using cremation can cost anywhere from $500 to $2,000. The less expensive version would entail only a cremation and a scattering of the ashes in an appropriate location. This would also mean no services and no memorialization and no urn. The more expensive version might entail a funeral service or memorial service, an expensive urn and memorialization in a cemetery.
Cremation is forbidden by Orthodox Judaism, the Eastern Orthodox Church and Islam. The Roman Catholic Church has allowed cremation since 1963 as long as traditional ceremonies respecting the body for purposes of resurrection are maintained. The ashes cannot be scattered or kept in the home but must be buried or entombed. Some Protestants allow cremation, some discourage it and others take no position.
Funeral Services and Funeral Service Providers
Probably the most common arrangement for closing out the life of a loved one is to have a funeral service and a burial in a local cemetery. Ostensibly funerals are touted as a way to honor the person who has passed away but in reality funerals are for the surviving family. The funeral is part of the mourning process. If the family has been proud of their loved one or if the loved one has had some standing in the community such as being a scholar, a doctor, a lawyer, a politician, a church leader or someone famous, the family wants the community to recognize their family member. They want to "show off" the deceased. As a general rule, the greater the status the more lavish the funeral. This recognition from the community and the emotional support from those who attend, in turn, help the family cope with the loss of their loved one. Here's an excerpt from the national Funeral Directors Association about funerals.
"Funerals fill an important role for those mourning the loss of a loved one. By providing surviving family members and friends a caring, supportive environment in which to share thoughts and feelings about the death, funerals are the first step in the healing process.
The ritual of attending a funeral service provides many benefits including:
• Providing a social support system for the bereaved.
• Helping the bereaved understand death is final and that death is part of life.
• Integrating the bereaved back into the community.
• Easing the transition to a new life after the death of a loved one.
• Providing a safe haven for embracing and expressing pain.
• Reaffirming one's relationship with the person who died.
• Providing a time to say good-bye."
If the deceased person was not respected by the community or the family, it is less likely that a formal funeral service will be held. But it is also possible that regardless of the status of the person who has died, the family may not want a public viewing and service because they do not want the attention of the community. Oftentimes they will simply have a burial service at the grave site for a very select number of people. Or they may choose cremation and scatter the ashes in a private ceremony somewhere that would have been special to the person who died.
Concerns from consumer groups that funeral homes or undertakers were taking advantage of family and asking them to make purchase decisions when they were most vulnerable to manipulation, after the death of a loved one, led to the Federal Trade Commission publishing rules for the sale of funeral services.
The Funeral Rule prohibits specific misrepresentations in the areas below (FTC 1997):
- Embalming - Funeral homes may not tell consumers that embalming is required unless a specific state or local law requires it. In MOST STATES, embalming is not required by law.
- Casket for Direct Cremation - Funeral homes cannot tell consumers that state or local law requires them to buy a casket if they are arranging a direct cremation for the cremation itself or for any other reason. An alternative container must also be made available.
- Outer Burial Container - Funeral homes cannot tell consumers that they are required to buy an outer burial container, unless a specific state or local law requires it. They also must tell consumers that state law does not require them to purchase an outer burial container.
- Legal and Cemetery Requirements - Funeral homes cannot tell consumers that any federal, state, or local law or particular cemetery or crematory requires them to buy a particular good or service, if that is not true.
- Preservative and Protective Value Claims - Funeral homes cannot make any representations to consumers that funeral goods or services will delay the natural decomposition of human remains for a long term or an indefinite time.
- Cash Advance Items - If funeral homes mark-up the charge on cash advance items or receive a commission, discount, or rebate that is not passed on to the consumer, they cannot state that the price charged for the cash advance item is the same as its true cost. This rule, however, does not prevent them from adding a service charge, nor does it require them to disclose the amount of that charge to the consumer.
Other Misrepresentations--other kinds of misrepresentations, though not specifically prohibited by the Funeral Rule, are nonetheless illegal. The FTC Act prohibits deceptive acts or practices. Likewise, the consumer protection laws of each state prohibit deceptive practices. The federal rule does not apply to businesses that sell funeral services only (cremation as an example) or goods only (caskets or grave markers as an example).
In times past family organized the funeral and the burial themselves. An undertaker may have been used for preparing the body for burial, providing a casket and providing a hearse to transport the body to a cemetery. Modern day funeral homes have made the arrangements more convenient, but also much more expensive. The funeral home or funeral director can handle everything from
- picking up the body after death,
- securing the death certificate,
- providing embalming,
- providing restoration services,
- printing funeral programs, sending invitations, providing guest books, etc.
- providing space for viewings and funeral services,
- submitting obituaries,
- obtaining required permits,
- making claim for Social Security or veterans benefits,
- providing a casket,
- securing cemetery lots,
- roviding outer burial chamber, liner or vault,
- providing transportation to the cemetery,
- moving the flowers from the funeral to the grave,
- arranging for the opening of a grave,
- making arrangements for a graveside burial service,
- arranging for closing the grave
- making arrangements for grave markers
- and possibly more.
Any of these services might be bought separately and the family could make arrangements for the balance or forgo such things as viewings, embalming and restoration, but it is more common the family will buy a "full service package" which includes all or most of the services outlined above.
As a general rule family-owned funeral homes or mortuaries are in the business of providing trusted service to members of their community. There may be a few that take advantage but by and large integrity is an important part of most providers' operations. Funeral directors have responded to criticism of their industry of pushing people into expensive and elaborate funeral services by providing more of the low cost services some families may desire. Not only do they offer cremation or simple burial without trying to pressure families, into more costly programs, but a recent trend has been to offer memorial services instead of an elaborate funeral. With a memorial service there is no viewing, no embalming, usually no flowers except maybe a few at the grave and there is a simple service designed to memorialize the departed loved one. The service can be held at the grave site or it can be held at a suitable meeting place later during the day or a few days following the burial. A memorial service can save considerable money over a traditional funeral.
Some groups feel that funeral directors monopolize the business of final arrangements for the dead and that they might be crowding out competition or influencing state legislatures to ban other types of similar services. The concern is that by discouraging competition, funeral homes can charge more money than is reasonable for their services. In fact eight states require using a mortuary for funeral arrangements if a casket is involved. In these states only funeral homes are allowed to sell caskets.
There is also concern that individual funeral homes are being purchased by large corporations and the public is not aware of this, since the original business name will be retained. As a general rule people have more trust in the local family-owned mortuary than in a faceless corporation. Funeral directors or morticians are often highly respected citizens in the community. By owning all of the funeral service providers in a given area, the corporation essentially has no competition from other homes and can charge higher prices for services. The recommendation is to check prices and plans before picking a particular funeral provider. Federal law requires them to give consumers accurate, detailed and itemized quotes over the phone. In 42 states there are other alternatives to a funeral home or mortuary.
In those states where market forces prevail, a call to several funeral service providers in the area will demonstrate that the family may not have to pay $5,000-$10,000 for a funeral. Some competitive providers don't follow the funeral home model, with fancy showrooms, beautiful hallways, very expensive caskets and lavish chapels or meeting rooms. They simply provide the services such as placing the body in the casket and transporting it to a burial site or arranging for cremation. It is up to the family to take care of the rest of the details. These companies may provide help with organizing a funeral or in dealing with the cemetery but these businesses are more often oriented towards selling caskets at competitive prices and providing guidance with the rest of the final arrangements.
In fact some companies only sell caskets as the casket is usually the largest single cost of a funeral. The "funeral rule" requires funeral homes to accept caskets from any source, not just their own. So a family can save money purchasing a casket from a casket dealer and using a mortuary to provide the other services. Caskets can also be ordered over the Internet. There are also many local artisans that will fashion caskets and sell them directly to the public at very reasonable prices. A list of these can be found on the Internet by searching for "caskets".
Alternate providers of funeral items and services can be found in the Yellow Pages under the headings "funeral homes", "funeral information" or "funeral services". Many of these service providers may offer funeral services in the range of $1,500 to $3,000.
In response to what they consider abusive pricing in the funeral industry, some consumers have organized nonprofit memorial societies. There are memorial societies in most states and they can be located in the Yellow Pages under the categories of "funeral homes" or "funeral information". Or they can be located on the Internet. These groups provide consumer counseling and written advice on alternatives to using high cost, funeral home "package" plans.
- They will provide documents and instructions for preplanning funeral arrangements
- They will provide reasons for not embalming.
- They will provide lists of reliable and low cost undertaker services.
- They will give reasons and instructions for cremation.
- They will give advice on where to go for quality caskets or basic funeral plans at a reasonable price.
- They will provide instructions on conducting memorial services instead of funerals.
- They may provide numerous low cost package programs as an alternative to using a funeral director to arrange these options
Social Security will pay $255 to be used towards a burial. It's important to follow up and apply for Social Security burial benefits even though it's not a lot of money. The Veterans Administration will also provide cemetery space for veterans. If the veteran's family can't afford a cemetery plot the VA will provide one in a veteran's cemetery. The VA will also pay for opening and closing the grave, for a standard marker and for the burial itself.
The Cemetery, a Place for Memorialization
In earlier times when our country was mostly rural, loved ones were often buried in a special area reserved for family near the family home or on the family property. And generally people in rural areas can still exercise this option. Today, where most people live within the boundaries of a government community, burying a loved one on one's property would not be allowed. A cemetery is the only option for interment of a body or the secure storage of one's ashes.
A cemetery is a place where one can go to remember loved ones. The grounds and markers are designed to create a memorial to people who have passed on. Larger cemeteries often have well-kept trees and lawns and perhaps even sidewalks or benches. They are typically in neighborhoods that are quiet and if a family member wants to spend some time there the environment is conducive to that.
The concept of providing a memorial to someone who has died is fundamental to humanity. All cultures past and present have some way of identifying a place to remember loved ones by. This is also an important part of providing closure for the grieving process--to have a place to identify our loved ones with. One of the problems with scattering ashes in a public place or over a body of water is that there is often no ability to identify that place and memorialization cannot take place. It may be important to some members of the family to have a special place. Cemeteries make allowances for cremations by providing places where urns can be placed. Some cemeteries also have special garden areas that allow for scattering of ashes. A memorial plaque can also be installed reminding the family where the ashes were scattered.
Wealthy rulers, politicians, people of status and rich people are the most ostentatious in having memorials in their honor. Consider the pyramids as an example. But even in local cemeteries it seems that families compete with each other by trying to erect grave markers or monuments that are better than the ones around them. Some cemeteries recognize this tendency and will restrict the size or design of grave monuments.
Probably the most important thing to remember in picking a cemetery is picking out a location that makes it convenient for the survivors to visit in the future. A cemetery halfway across the country that is picked simply because it was the birthplace of the decedent is not being considerate to the family that may be hundreds of miles away. On the other hand if family are scattered all over the country, location may not be a problem. A second important consideration is also a convenience issue. Many families have parents, grandparents, aunts and uncles and children buried in the same cemetery. This makes it convenient for family members who want to remember more than one loved one to do so by visiting only one location. The cemetery where the rest of the family is buried should be the logical choice. Oftentimes a person will pick his or her cemetery plot based solely on the atmosphere of the place and not take into account the convenience issues expressed above. Being considerate to the surviving family is an important issue in picking a cemetery.
There are presently two types of cemeteries. The first is the traditional cemetery that has been used for perhaps hundreds of years and is filled with upright monuments of stone or above ground mausoleums. The second is a newer concept called a memorial park or memorial garden. This is an effort to equalize everyone who is buried by not allowing any one family to erect monuments different from anyone else. The only markers allowed are ground level tablets of a prescribed size. The Memorial Park is designed to resemble a garden where people can repose or reflect in beautiful surroundings. There may be fountains, sculptures, inviting buildings, water features and so on. Some cemeteries use both concepts.
Here are some issues to consider or issues to generate questions to ask when buying a cemetery plot when preplanning funeral arrangements.
- The plot is not owned, only the usage of the plot for a perpetual interment.
- Prices will vary considerably but generally be more expensive in urban areas with high land values and less expensive in rural areas.
- If a plot is purchased but the family desires another cemetery instead, many cemeteries have exchange programs where the equivalent values can be exchanged between cooperating cemeteries, but many cemeteries do not have exchanges or the exchanges may not work as advertised and the family may be stuck with an unwanted cemetery lot.
- Some cemeteries may be willing to repurchase plots.
- Grave liners or vaults are not required by law but some cemeteries may require them to prevent the ground from sinking.
- Generally plots cannot be resold privately to another individual.
- Most cemeteries that sell memorials place restrictions on the installation of memorials purchased elsewhere. This limits the consumer's choice and drives up the price.
- Most cemeteries will only allow their own personnel to open and close graves.
- Cemeteries may use high-pressure tactics to get people to make a decision on the spot.
Pre-planned Final Arrangements with No Formal Funding
Laws in all states generally hold that funerals benefit the survivors and the person who has died has very little to say in the manner in which services are provided for his or her final interment. In most states a person can express the method of final arrangements in a will but in reality, unless there is a sizable estate and the division is contingent upon probating the will, very few families actually execute a will in probate court. Even if there is a will at death, there is usually no reason to respect it, since most personal assets and savings have been transferred in fact, through beneficiary arrangement or by default to the survivors and the home may pass by joint tenancy, by separate probate or in a trust. Most often wills are never used and remain at home in the drawer or in a safety deposit box.
This does not mean; however, that someone can't plan in advance for his or her funeral. There are reasons that people want to plan in advance.
- They have been through final arrangements with their own loved ones and experienced stress in making decisions dictated by time constraints.
- They have been concerned with what the loved one would have wanted for his or her final arrangements.
- They have been troubled by how much they should spend and not be considered spendthrift's by those who attend the funeral.
- Or they have wondered if the choice of funeral speakers, music and other recognition rituals had been what the loved one would have appreciated.
As a result, many older people want to spare their own family the stress they went through in burying their loved ones. They want to plan in advance for their funeral.
The person planning final arrangements provides a written plan for the family and possibly for a trusted funeral service provider outlining the details of what is to happen. A family meeting is arranged and an agreement is reached that the family will respect these last wishes. However, this is not a legal arrangement. Money can be set aside for this plan or the family may find money from other sources. If there is permanent life insurance, a portion or all of those proceeds can also be used to pay for the services and goods. The funeral services provider agrees to follow through with the plan upon approval of the family after the death. The following issues should be considered when designing a pre-arrangement plan.
- If a funeral service provider is selected in advance, will that provider offer similar services in the future, try to pressure the family to "buy up" to more expensive options or even be in business?
- Will the desired funeral items such as caskets, vaults or liners or grave markers be available in the future? If not, are contingency plans provided?
- About half of the states allow a disposition authorization form to be signed before death choosing cremation or burial as a final disposition. This bypasses approval by the family. If you live in such a state and you want this provision have you checked with your funeral service provider for availability of signing the form now?
- If there is no pre-arrangement with a service provider, will the family know how to properly shop for a funeral?
- In some states, if cremation is desired, all family members must agree. Has this been worked out before hand?
- Where will the money come from to provide for the funeral and burial and if it is to come from savings or insurance, has enough been set aside to allow for inflation with future costs?
- Is the funeral program flexible enough to allow for participants who may not be available at the time of the funeral?
- Do all family members agree on the price range or will one person bolt and insist on spending more?
- If a nonpublic interment with no viewing, no services, no flowers and no fancy caskets is desired will the family respect this request?
- If the person having preplanned, moves to another state is there a contingency plan?
About half of all states recognize the right of the deceased to pick the final disposition of the body -- either burial or cremation. In those states with no disposition laws, courts will likely recognize a written declaration by the decedent on his or her preference for disposition especially if the document came from a state that had a disposition law. Some states allow appointment of a designated agent for body disposition. This is most useful as it provides someone who can represent the interests of the person making the request after death occurs.
One way to informally provide future funds for a prearranged funeral and burial is to buy a life-insurance policy specifically designed for this purpose. And of course anyone who has an existing life-insurance policy that is a permanent contract -- will not lapse at some future date -- can use all or a portion of that death benefit to pay for future funeral costs. Traditional life insurance policies are generally designed for younger people who are in reasonably good health. In addition these policies are usually not available in amounts less than $50,000 in face value. Older people may qualify for these policies, but many elderly who are in good health may not want to buy a policy that large since it could be very expensive. Some life insurance companies specialize in permanent life insurance burial policies for older ages and for people with health problems.
These so-called "final expense" policies are designed to accommodate smaller amounts of death benefit and people who might normally be uninsurable through traditional policies. Available death benefits may range from $2,500 to $50,000. As an example, for a 65-year-old in reasonably good health, a permanent policy with a $10,000 death benefit might cost about $42 to $87 a month depending on the gender and smoking habits of the applicant. The policy will generally have cash value after a certain number of years and may also increase in death benefit value in future years. For those who have cancer or heart disease or life-threatening health problems or in some other way may be uninsurable there are so-called "guaranteed issue" policies. A $10,000 policy like this for a 65 year old might cost $75 to $87 a month depending on gender. In order to protect itself from too many premature death claims with guaranteed issue policies, the insurance company usually has some kind of a waiting period on these policies before a benefit will be paid. One arrangement might pay nothing if death occurs in the first six months, 50% of the death benefit in the second six months, and the full death benefit after the first year. Another policy might simply exclude payment for any death claim in the first two years. This policy would probably be less expensive than the one quoted above.
A major problem with final expense policies is that overhead costs, claims, commissions and other costs associated with managing these contracts make premiums much higher in proportion to death benefit than with larger policies of $100,000 or more. Final expense policies are also generally designed to be more lenient in covering the death of policyholders who may have major health problems. And those final expense policies that guarantee coverage regardless of health are obviously going to pay out death claims sooner than a policy that required someone to be in good health when they applied. All of these factors make final expense policies very expensive relative to the death benefit.
Someone in good health buying one of these policies could live a long time. Premiums are generally set up to be paid monthly or yearly as long as the person lives. Some people living a long time and paying into one of these policies could end up paying significantly more in premiums than the policy would pay at death. Such a policy is only a good idea if a person is in poor health and not expected to live very long. For someone in good health, putting money away in a savings account is usually a better option.
Some people use a memorial society to help with preplanning funeral arrangements. One popular group is the Funeral Consumers Alliance which has affiliates in most states. Memorial societies can be found by looking under funerals in the Yellow Pages or local affiliates can be found by going to www.funeral.org.
PreNeed (Pre-Paid) Funeral and Burial Plans
Advantages and Disadvantages of Prepaid Plans
Another way to plan in advance is to sign a formal contract called a "preneed funeral plan", where money is held in a trust, in an escrow account or paid through an insurance policy. Parts of or all of the funeral service and burial are designed in advance and prefunded in advance and the family has little to do but show up. This type of planning has become very popular in recent years. A survey conducted by the AARP in 1999, found that two out of five people over age 50 had been approached to pre-purchase funerals and burial goods and services. An AARP survey in 1998 indicates that 32% of all Americans over age 50, roughly 21 million people, have prepaid some or all of their funeral and or burial expenses (but not necessarily through a formal preneed plan). Breaking that down, about 25% of the over age 50 population have prepaid for their burials (cemetery plot, mausoleum or niche), 18% have prepaid for headstones, urns, caskets , grave liners or vaults, opening and closing of graves and so on and 13% have prepaid for goods or services from a funeral home or funeral director. The same article indicates that over $25 billion is being held in pre-need trust funds. Roughly another $25 billion is waiting to be paid out in life insurance benefits. Prepaid or preneed funerals and burials are big business.
Prepaid funerals and burials funded privately by the family, or paid from an individual life insurance policy and arranged informally through a funeral home or funeral director, are generally not subject to state regulation. Any formal arrangement through a second party or involving a contract is subject to regulation in all states. Each state has adopted different rules as to who can sell these plans, what the plans can provide, what contract provisions must be, how the plan is to be on funded and what recourse purchasers might have in the event of fraud or default. All states call these regulated plans "preneed" funeral and burial arrangements.
ere are some advantages to why one would want to buy a preneed plan for funeral and burial services and goods.
- It provides peace of mind knowing these arrangements have been made in advance
- It avoids the burden on family members to make decisions when they are most vulnerable to manipulation.
- It allows one to virtually control from the grave by determining in advance the funeral products, funeral services, burial products and burial services that one would prefer having for final arrangements.
- It helps the family to avoid taking loans, arranging finance plans, raiding savings or selling assets to pay for a funeral and burial.
- It guarantees (for many contracts) that if products and services currently purchased are not available in the future, equivalent substitutes will be provided at no additional cost.
- It locks in guaranteed prices (available with some contracts) forever.
- It allows for inflation in future costs (for those contracts that do not guarantee prices) by investing money in an interest-bearing account or buying life insurance that increases in value over time.
- Depending on the contract, it may allow for transfer to another funeral home or for partial or full refund.
Unfortunately, there are also problems with prepaid, preplanned final arrangements.
- With some trust fund and insurance funding options there may be no refund if someone wants to cancel the plan in the future.
- If a purchaser moves to another state there may be no transfer options or there may be different rules governing the funding option.
- In some contracts, interest earnings on investments resulting in excess money not needed for the plan may be retained by the funeral home or funeral director.
- On installment plans interest may be charged but not credited to the account.
- In certain insurance funded contracts, the ownership or death benefit may be irrevocably assigned to the contract holder, preventing the purchaser from enjoying ownership rights in the policy.
- In certain insurance funded contracts, a growth in the death benefit over time that exceeds the cost of the pre-need plan services and goods may be pocketed by the contract holder instead of being refunded.
- If the contract provider goes out of business or fails to secure 100% of the funds for future payment, there may be no recourse to get all of the money back that was put in.
- If certain services or goods that were purchased initially are not available in the future, but more expensive versions might be, the family may be forced to pay extra for those items.
- In certain insurance funded plans, if the insured dies too soon, there may have been a waiting period in which few or no benefits are paid at death, thus forcing the family to pay out of pocket for the funeral.
- Certain unscrupulous providers may have failed to provide an itemized list of services and goods or failed to identify properly, specific services and goods, thus allowing the provider in the future to substitute less expensive items or to leave out services and goods that were originally anticipated in the agreement.
What Services and Goods Can Be Prepaid?
All states allow for prepaid plans for funeral services and merchandise. This would include such things as picking up the body, embalming and restoration, rooms or chapel for viewing and funeral services, casket, vault or grave liner, transportation, permits, death certificates, obituaries and so forth. Almost all states allow for prepaid burial services and merchandise as well. Only about six states do not allow it. Burial services and merchandise might include opening and closing the grave, grave markers, vaults or grave liners, mausoleums or niches. Cemetery plots are excluded from prepaid plans in all states.
Who Can Sell These Plans?
In 16 states, anyone with a special license can sell preneed funeral plans. About the same number of states allow special license sales of preneed burial plans. If the preneed sale involves insurance, all states require an insurance license as well. Most states generally restrict sales to funeral homes, or funeral home directors or their employees or agents. Again if employees or agents sell insurance they also need to be insurance licensed
Most states allow for using life insurance for funeral plans and a large number of states allow it for burial plans. In those states that allow insurance, three or four insurance companies have designed policies specifically to fund preneed contracts.
A standard contract is used with all funeral providers in each state that may or may not guarantee the cost of goods and services and does not require irrevocable assignment of the death benefit to the funeral provider. Where allowed, the contract will include burial services as well.
Persons wanting a preneed contract will sit down with a Forethought agent, go over the various package plans available, choose the desired plan, apply for the insurance and sign the contract. A detailed description of services, merchandise and prices is given to the purchaser. The purchaser also agrees to provide a revocable assignment of death benefit on the policy to the funeral provider. Since the assignment of death benefit is revocable, the purchaser can walk away from the contract at any time and transfer that death benefit to another funeral home if desired. If the contract guaranteed prices, however, a new funeral provider may not except those prices and may charge more money.
How Are These Plans Funded?
About six states allow the use of an escrow account to hold money paid into a preneed arrangement. An escrow account is typically a bank trust account funded by the purchaser and managed for the contract provider. Four of these states also allow for at least one other funding option as well such as using a trust fund. Rhode Island and Connecticut do not.
Most states allow for a specially established trust fund to hold money for preneed arrangements for both funeral and burial plans. A trust fund must be managed by a third-party trustee. Banks often provide this service. The trust fund may be revocable -- meaning the purchaser can remove his money -- or irrevocable -- meaning the purchaser has no claim to the money. These options depend on state rules, on the contract or whether it is a Medicaid spend down trust. The purchaser may put the money in with a series of installment payments or may put the entire amount in within a short time of signing the contract. Most states require that at least 90% of the money destined to pay the preneed plan must remain in the trust. Some states allow the trust to be funded at a lesser percentage. Some states require 100% of the money must remain in the trust.
For those trusts that are partially funded, the money not invested can be spent by the funeral provider with the understanding that the provider will have to replace it when the purchaser dies. What this means for the purchaser is in those states which don't require 100% funding, if the provider has spent the money from this trust account as well as all other trust accounts it is using for prepaid plans, when the time comes to pay for services and goods, the provider may be short of cash and may be unable to pay the balance. A handful of states have recognized this problem and they assess all preneed providers a certain amount of money that goes into a consumer protection fund to reimburse the purchaser if the provider is unable to perform.
Most states allow for using life insurance for funeral plans and burial plans. Estimates are that about 70% of all preneed plans are funded with life insurance. Using Forethought Insurance again as an example, the company offers two kinds of insurance plans starting at an $800 death benefit amount and not exceeding a $25,000 death benefit. The first policy is a guaranteed issue policy -- meaning no health questions are asked -- that is paid up either in one lump sum payment, or with three years of payments, or five years of payments or 10 years of payments. With the single sum payment policy, if the insured dies before six months, the single sum plus interest is returned. After six months the death benefit is paid in full. With the three and five-year payment policies, if the person dies before one year, premiums plus interest are returned. After one year, percentages of the full death benefit are paid based on an increasing scale each year until 100% of the death benefit is reached. With the 10-year paid-up policy the insured must wait two years before the death benefit is paid and the year-to-year increasing scale of benefits also applies. Except for the 10 year paid-up plan, none of this company's insurance plans result in an insured paying in more than the initial death benefit of the policy. The policy death benefit also increases over time to keep pace with inflationary costs of services and items if the preneed contract is not price guaranteed. Increases in death benefit are dependent upon interest earnings and other factors and are not guaranteed.
The major problem with these policies other than the single pay policy are a risk that if a person dies shortly after getting the policy, there is no death benefit to pay for the prearranged funeral plans. On the other hand, the family is not out any money because premiums plus interest are returned. It means the family now must come up with a lump sum of money that would have come instead from an insurance policy death benefit. Since the single sum payment policy will be fairly close to the actual death benefit, the return of that premium will mostly cover the cost of the preneed plan. Forethought estimates that about 70% of its policies are paid with one single sum.
The other type of Forethought Insurance policy is for people whose health might permit them to buy a cheaper premium in proportion to the death benefit. With this policy the insured gets more death benefit for less money. This policy asks for a person's health history and goes through an "underwriting" process where the company determines if it can accept an immediate risk on the potential death of the applicant. If the applicant is approved, the death benefit is in effect as soon as the policy premium has been paid. All policies provided by Forethought increase in value over time and when the insured dies the excess not used to pay the preneed plan is refunded to the insured's family.
One advantage to the Forethought contract and policy is that preneed costs may in many cases be guaranteed. Another advantage is the policy does not need to be irrevocably assigned to the funeral home. In essence the policyholder can designate whomever he or she wants to receive the death benefit. This in turn makes the contract conditional because nothing has been given to the provider in return for services and goods. This also means the contract holder can walk away from the contract at any time. The problem is the purchaser may end up losing a cost guarantee if he or she tries to use the insurance to set up a new plan with another funeral home. The new funeral home is not required to honor the previous contract but may do so.
How Are Consumers Protected from Fraud or Default?
We've already discussed consumer protection funds in eight states that are designed to repay the purchaser if the funeral provider cannot replace monies used in trust funds. A number of states allow for a full refund upon cancellation, including interest, as long as the preneed contract was revocable and the purchaser followed all provisions for obtaining the refund. A handful of states allow further legal recourse to purchasers either under the state's Unfair and Deceptive Acts and Practices Law, or by allowing consumers who have been injured to file a civil action in state court.
Anyone buying a contract from a provider who is a member of the National Funeral Directors Association receives the following guarantees:

Prepaid Trust Plans for Medicaid Spend Down
Medicaid rules allow someone going through a Medicaid spend down -- in order to have Medicaid pick up all or part of their nursing home bill -- to retain $1,500 for funeral expenses. For many that is not enough. Most states allow potential Medicaid recipients going through spend down to put up to an additional $7,000 or possibly more, with allowances for burial expenses, into an irrevocable funeral and burial plan. Preneed plans are most often used with this spend down provision. Money must be put into a trust arrangement where the trustee will pay for funeral costs and burial costs after the death of the trust owner -- the purchaser. The trust must be irrevocable meaning the purchaser of the preneed plan has no claim on the money or interest earnings. If insurance is used for funding, the ownership of the policy or the death benefit must be irrevocably assigned to the trust. Some states may not allow insurance to be used in this type of trust. Neither cash value nor the death benefit is available to the family. Purchasers who have entered into irrevocable funeral and burial trusts may only use the funds for payment of funeral services and merchandise upon the death of the intended funeral recipient. Any excess in the trust account after payment of funeral expenses might go back to Medicaid or be returned to the local county Social Services Department in which the intended funeral recipient resided, to be earmarked for indigent burials.
Federal law protects the beneficiaries of Medicaid funeral trusts. The law allows the consumer to change funeral homes at any time prior to death without affecting the irrevocability of the arrangements themselves. If such a transfer is desired, a new irrevocable preneed agreement with the newly selected funeral home must be generated. The transfer of irrevocable preneed funds may, however, ONLY be made payable to another funeral home, or another funeral trust program.
Additionally, the law permits the beneficiary's family, at the time of need, to select different goods and services from those originally prearranged. Please note, however, that the funds in the account may only be used for payment of funeral services and merchandise. Any remaining funds in the account after payment of funeral services and merchandise must be remitted by the funeral director to the appropriate trust designated government recipient. The money cannot go back to the family.
Checklists and Contact Information
The AARP has excellent information for consumers on planning for funerals. Here's an excerpt from the AARP web site at https://www.aarp.org/families/grief_loss/
"Most states have a licensing board that regulates the funeral industry. You may contact the board in your state for information or help. If you want additional information about making funeral arrangements and the options available, you may want to contact interested business, professional and consumer groups. Some of the biggest are:
AARP Fulfillment
601 E Street, NW Washington, DC 20049
1-800-424-3410
www.aarp.org
AARP is a nonprofit, nonpartisan organization dedicated to helping older Americans achieve lives of independence, dignity and purpose. Its publications, Funeral Goods and Services and Pre-Paying for Your Funeral, are available free by writing to the above address. This and other funeral-related information is posted on the AARP website.
Council of Better Business Bureaus, Inc
4200 Wilson Blvd., Suite 800 Arlington, VA 22203-1838
https://www.bbb.org/alerts/article.asp?ID=162
Better Business Bureaus are private, nonprofit organizations that promote ethical business standards and voluntary self-regulation of business practices. The BBB's website offers information about pre-need funeral planning.
Funeral Consumers Alliance
PO Box 10 Hinesburg , VT 05461
1-800-458-5563
www.funerals.org
FCA, a nonprofit, educational organization that supports increased funeral consumer protection, is affiliated with the Funeral and Memorial Society of America (FAMSA).
Cremation Association of North America
401 North Michigan Avenue Chicago , IL 60611
(312) 321-6806
www.cremationassociation.org
CANA is an association of crematories, cemeteries and funeral homes that offer cremation.
International Cemetery and Funeral Association
1895 Preston White Drive, Suite 220 Reston, VA 20191 1-800-645-7700
www.icfa.org
ICFA is a nonprofit association of cemeteries, funeral homes, crematories and monument retailers that offers informal mediation of consumer complaints through its Cemetery Consumer Service Council. Its website provides information and advice under "Consumer Resources."
International Order of the Golden Rule
13523 Lakefront Drive St. Louis , MO 63045
1-800-637-8030
www.ogr.org
OGR is an international association of about 1,300 independent funeral homes.
Jewish Funeral Directors of America Seaport Landing
150 Lynnway, Suite 506 Lynn , MA 01902
(781) 477-9300
www.jfda.org
JFDA is an international association of funeral homes serving the Jewish community.
National Funeral Directors Association
13625 Bishop's Drive Brookfield , WI 53005
1-800-228-6332
www.nfda.org/resources
NFDA is the largest educational and professional association of funeral directors.
National Funeral Directors and Morticians Association
3951 Snapfinger Parkway, Suite 570 Decatur , GA 30035
1-800-434-0958
www.nfdma.com
NFDMA is a national association primarily of African-American funeral providers.
National Selected Morticians
5 Revere Drive, Suite 340 Northbrook , IL 60062-8009
1-800-323-4219
www.nsm.org
NSM is a national association of funeral firms that have agreed to comply with its Code of Good Funeral Practice. Consumers may request a variety of publications through NSM's affiliate, the Consumer Information Bureau, Inc.
Funeral Service Consumer Assistance Program
PO Box 486 Elm Grove , WI 53122-0486
1-800-662-7666
FSCAP is a nonprofit consumer service designed to help people understand funeral service and related topics and to help them resolve funeral service concerns. FSCAP service representatives and an intervener assist consumers in identifying needs, addressing complaints and resolving problems. Free brochures on funeral related topics are available.
Funeral Service Educational Foundation
13625 Bishop's Drive Brookfield , WI 53005
1-877-402-5900
FSEF is a nonprofit foundation dedicated to advancing professionalism in funeral service and to enhancing public knowledge and understanding through education and research.
Planning for a Funeral
|
Make copies of this page and check with several funeral homes to compare costs
"Simple" disposition of the remains: |
|
|
|
Immediate burial |
__________ |
|
Immediate cremation |
__________ |
|
If the cremation process is extra, how much is it? |
__________ |
|
Donation of the body to a medical school or hospital |
__________ |
|
|
|
"Traditional," full-service burial or cremation: |
|
|
|
Basic services fee for the funeral director and staff |
__________ |
|
Pickup of body |
__________ |
|
Embalming |
__________ |
|
Other preparation of body |
__________ |
|
Least expensive casket |
__________ |
|
Description, including model # |
__________ |
|
Outer Burial Container (vault) |
__________ |
|
Description |
__________ |
|
Visitation/viewing - staff and facilities |
__________ |
|
Funeral or memorial service - staff and facilities |
__________ |
|
Graveside service, including staff and equipment |
__________ |
|
Hearse |
__________ |
|
Other vehicles |
__________ |
|
Total |
__________ |
|
|
|
Other Services: |
|
|
|
Forwarding body to another funeral home |
__________ |
|
Receiving body from another funeral home |
__________ |
|
|
|
Cemetery/Mausoleum Costs: |
|
|
|
Cost of lot or crypt (if you don't already own one) |
__________ |
|
Perpetual care |
__________ |
|
Opening and closing the grave or crypt |
__________ |
|
Grave liner, if required |
__________ |
|
Marker/monument (including setup) |
__________ |
Glossary of Terms
(Courtesy of the California Department of Consumer Affairs, Cemetery and Funeral Bureau)
Alternative Container An unfinished wood box or other non-metal receptacle without ornamentation, often made of fiberboard, pressed wood or composition materials, and generally lower in cost than caskets.
Casket/Coffin A box or chest for burying remains.
Cemetery Property A grave, crypt or niche.
Cemetery Services Opening and closing graves, crypts or niches; setting grave liners and vaults; setting markers; and long-term maintenance of cemetery grounds and facilities.
Columbarium A structure with niches (small spaces) for placing cremated remains in urns or other approved containers. It may be outdoors or part of a mausoleum.
Cremation Exposing remains and the container encasing them to extreme heat and flame and processing the resulting bone fragments to a uniform size and consistency.
Crypt A space in a mausoleum or other building to hold cremated or whole remains.
Disposition The placement of cremated or whole remains in their final resting place.
Endowment Care Fund Money collected from cemetery property purchasers and placed in trust for the maintenance and upkeep of the cemetery.
Entombment Burial in a mausoleum.
Funeral Ceremony A service commemorating the deceased, with the body present.
Funeral Services Services provided by a funeral director and staff, which may include consulting with the family on funeral planning; transportation, shelter, refrigeration and embalming of remains; preparing and filing notices; obtaining authorizations and permits; and coordinating with the cemetery, crematory or other third parties.
Funeral Planning Society See Memorial Society.
Grave A space in the ground in a cemetery for the burial of remains.
Grave Liner or Outer Container A concrete cover that fits over a casket in a grave. Some liners cover tops and sides of the casket. Others, referred to as vaults, completely enclose the casket. Grave liners minimize ground settling.
Graveside Service A service to commemorate the deceased held at the cemetery before burial.
Interment Burial in the ground, inurnment or entombment.
Inurnment The placing of cremated remains in an urn.
Mausoleum A building in which remains are buried or entombed.
Memorial Service A ceremony commemorating the deceased, without the body present.
Memorial Society An organization that provides information about funerals and disposition, but is not part of the state-regulated funeral industry.
Niche A space in a columbarium, mausoleum or niche wall to hold an urn.
Urn A container to hold cremated remains. It can be placed in a columbarium or mausoleum, or buried in the ground.
Vault A grave liner that completely encloses a casket.
You can file a complaint with the FTC by contacting the Consumer Response Center by phone: toll-free 1-877-FTC-HELP (382-4357); TDD: 202-326-2502; by mail: Consumer Response Center, Federal Trade Commission, 600 Pennsylvania Ave, NW, Washington, DC 20580; or through the Internet, using the online complaint form. Although the Commission cannot resolve individual problems for consumers, it can act against a company if it sees a pattern of possible law violations.
The FTC publishes free brochures on many consumer issues. For a complete list of publications, write for Best Sellers, Consumer Response Center , Federal Trade Commission, 600 Pennsylvania Ave, NW , Washington , DC 20580 ; or call toll-free 1-877-FTC-HELP (382-4357), TDD 202-326-2502."







